Revolutionary DNA Therapy Cuts LDL Cholesterol by Nearly Half – No Statins Needed
DNA-based molecules targeting PCSK9 reduce LDL cholesterol by nearly 50% without statins, offering a breakthrough alternative for heart disease prevention.
A groundbreaking development in cholesterol management has emerged, offering hope for millions who struggle with high LDL levels. Researchers have created tiny DNA-based molecules that target a specific protein responsible for keeping 'bad' cholesterol in the bloodstream. This innovative approach reduces LDL cholesterol by nearly 50% without relying on traditional statin drugs. Below, we answer key questions about how this therapy works, its effectiveness compared to statins, and its potential impact on heart disease prevention.
What is the new treatment and how does it work?
This novel treatment uses tiny DNA-based molecules designed to block the action of a protein called PCSK9. Normally, PCSK9 binds to LDL receptors on the surface of liver cells, causing them to be destroyed. This reduces the liver's ability to remove LDL cholesterol from the blood. By silencing the PCSK9 gene using these molecules—often referred to as antisense oligonucleotides or small interfering RNA—the production of the protein is halted. With less PCSK9, more LDL receptors remain active, allowing cells to absorb and break down LDL cholesterol instead of letting it accumulate in artery walls. This mechanism effectively lowers circulating bad cholesterol levels dramatically.
How effective is this approach compared to statins?
Clinical studies show that this DNA-based therapy reduces LDL cholesterol by roughly 50%, which is comparable to the reduction seen with high-potency statins. However, unlike statins, which work by inhibiting cholesterol production in the liver, this therapy targets the PCSK9 pathway—a more direct method of enhancing cholesterol clearance. Early results indicate it may be particularly beneficial for patients who cannot tolerate statins due to side effects like muscle pain or those with genetic conditions causing extremely high cholesterol. While statins remain a first-line treatment, this new option could serve as a powerful alternative or add-on therapy, potentially reducing the need for daily pills.
What role does PCSK9 play in cholesterol regulation?
PCSK9 (proprotein convertase subtilisin/kexin type 9) is a key regulator of LDL cholesterol levels. It acts as a 'gatekeeper' by binding to LDL receptors on liver cells and marking them for degradation. When PCSK9 is overactive, fewer receptors are available to remove LDL from the blood, leading to high cholesterol. Genetic mutations that overproduce PCSK9 are linked to familial hypercholesterolemia, a condition causing dangerously high LDL levels and early heart disease. Conversely, people with naturally low PCSK9 activity tend to have very low cholesterol and reduced cardiovascular risk. This makes PCSK9 an ideal target for therapies that aim to boost receptor availability and improve cholesterol clearance naturally.
Why is this considered a breakthrough in cholesterol management?
Traditional cholesterol treatments have relied heavily on statins, which, while effective, come with limitations such as muscle pain, liver enzyme elevations, and incomplete efficacy in some patients. The new DNA-based therapy represents a paradigm shift because it attacks cholesterol from a different angle—enhancing clearance rather than reducing production. Moreover, it uses synthetic nucleic acids to precisely silence a gene, a technique with broader implications for treating other conditions. The therapy's ability to lower LDL by nearly 50% without statins offers an alternative for the estimated 20% of patients who cannot take statins. It also opens the door to personalized medicine, where treatment can be tailored to an individual's genetic profile, particularly for those with PCSK9-related disorders.
What are the potential implications for heart disease prevention?
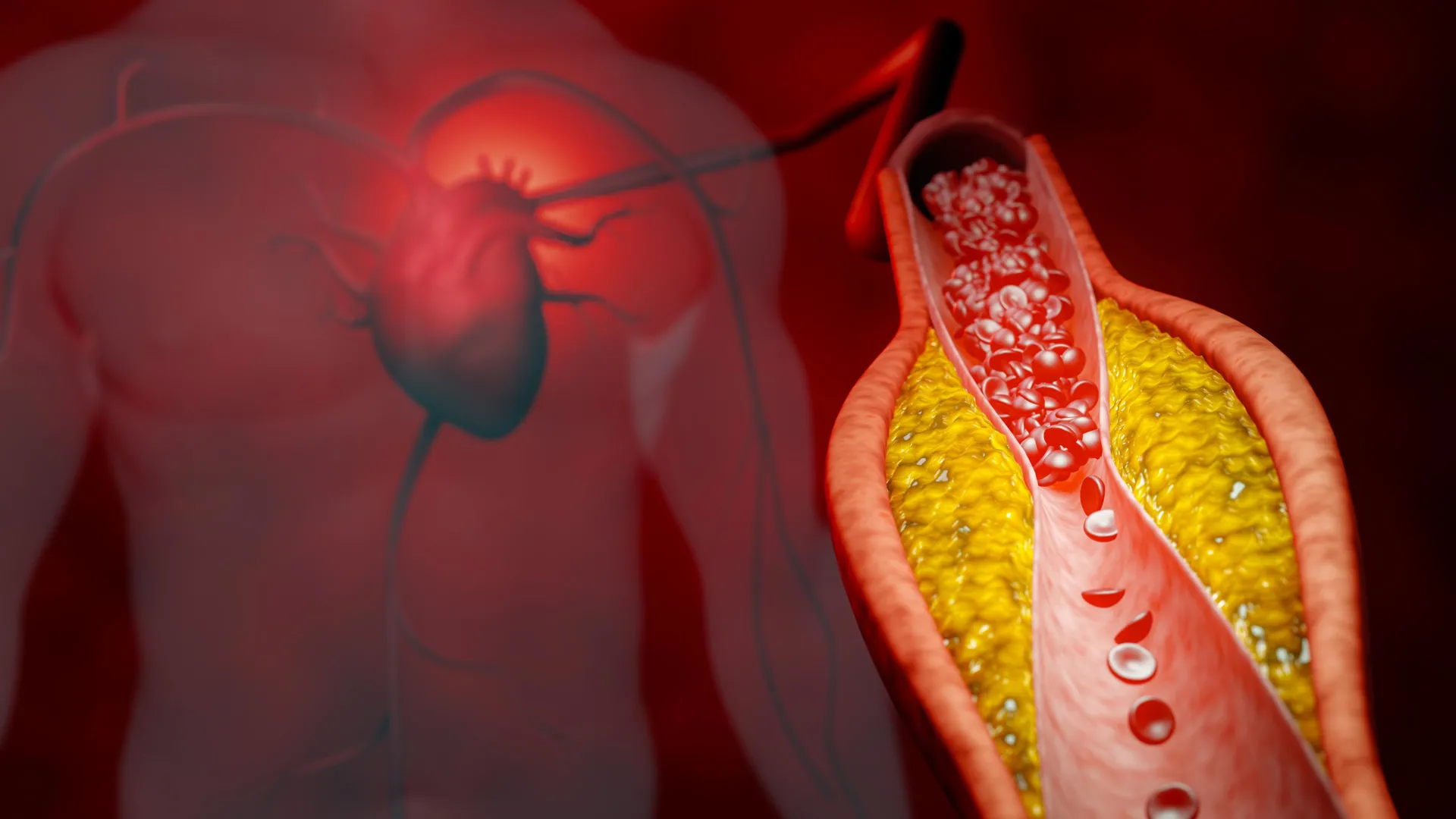
High LDL cholesterol is a major driver of atherosclerosis—the buildup of plaque in arteries that leads to heart attacks and strokes. By cutting LDL levels by half, this new therapy could significantly reduce the risk of cardiovascular events. In fact, studies have shown that for every 1 mmol/L reduction in LDL, the risk of major coronary events falls by about 20%. If the DNA-based molecules produce sustained reductions, they could prevent thousands of heart attacks annually. The therapy may be especially impactful for high-risk groups, such as those with diabetes, existing heart disease, or genetic conditions like familial hypercholesterolemia. Long-term trials are still needed, but the early data suggests a promising new weapon against the world's leading cause of death.
Are there any side effects or risks associated with this therapy?
Because the therapy is still in clinical development, a full safety profile is not yet established. Preliminary studies indicate it is generally well-tolerant, with common side effects including injection-site reactions like redness or swelling, mild flu-like symptoms, and occasional liver enzyme changes. Unlike statins, there have been no reports of significant muscle pain. However, because the molecules are synthetic and delivered via injection (often every few weeks), issues like immune responses or off-target effects are being monitored. Researchers are also assessing long-term safety, particularly regarding potential impacts on gene regulation. As with any new therapy, the benefits of dramatically lowering cholesterol must be weighed against these risks, and strict eligibility criteria will apply.
When might this treatment become available to patients?
As of now, the therapy is in Phase 2 and 3 clinical trials, the final stages before seeking regulatory approval from bodies like the FDA or EMA. If results continue to show strong efficacy and acceptable safety, approval could come in the next 3 to 5 years. However, the timeline depends on the successful completion of larger trials that evaluate cardiovascular outcomes, not just cholesterol levels. If approved, the therapy would likely be available by prescription, initially for high-risk patients or those intolerant to statins. Because it is an injectable biologic, it may be more expensive than daily pills, potentially limiting access until insurance coverage widens. Researchers are also exploring whether the molecules can be packaged into a oral formulation to improve convenience.